
A new report prepared for Health Canada shows that the legalization of cannabis in Canada in 2018 improved access, information sharing, and reduced stigma associated with cannabis for medical purposes.
The report is based on two surveys, one of 1,205 Canadians aged 16 and up who have used cannabis for medical purposes since it was legalized on October 17, 2018. The second survey was from a sample of 823 medical doctors and nurse practitioners who have had experiences with individuals accessing or inquiring about cannabis for medical purposes.
Of those individuals surveyed who used cannabis for medical purposes (“patients”), just over half (53%) reported doing so prior to legalization. Nearly half (46%) only began using cannabis for medical purposes after cannabis was fully legalized.
Of those who only began using cannabis for medical purposes after legalization in 2018, more than half (58%) said they were more comfortable doing so because legalization made cannabis easier to access. Half (49%) also said they made the decision to use cannabis for medical purposes because they felt more information on medical cannabis was available post-legalization and stigma was less of a factor.
Most (71%) of those who said they used cannabis for medical purposes reported also using cannabis for non-medical purposes in the past 3 years since legalization.
Most of these patients (66%) also said they had discussed their use of cannabis for medical purposes with a medical doctor and/or nurse practitioner. Of those who didn’t discuss these issues with a healthcare practitioner (HCP), fear of stigma was the most common reason.
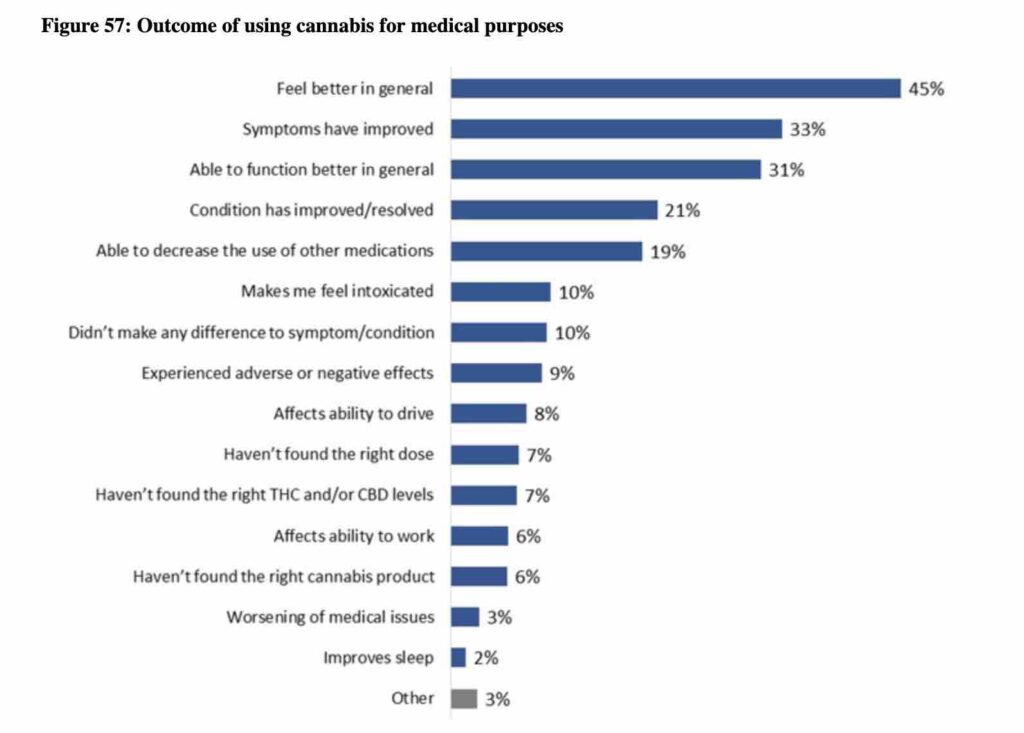
Of those who discussed medical cannabis with an HCP, more than half (53%) received a medical authorization document to access cannabis through the medical cannabis sales stream. Most patients who sought such authorization were given one by an HCP, and only 20% who asked were refused by their HCP.
Among those who received a medical document, the majority were either registered with a licensed seller or authorized to produce their own cannabis. About one-third (37%) did so through a licensed producer, while 33% grew their own cannabis. Another 13% were authorized to access through a designated grower.
The most common reasons for refusal were the HCP not being willing to authorize cannabis for patients (38%), a reported lack of evidence to support cannabis as a treatment option (31%), or that the HCP was not familiar enough with the use of cannabis for medical purposes (29%).
Types of cannabis products recommended
Cannabis oils, extracts, and capsules were the most commonly recommended product by a healthcare provider (68%), followed by edibles at 26% and dried flower at 23%.
Nearly one-third reported being recommended high-CBD and low-THC products, while 24% said they were recommended equal amounts of THC and CBD. Another 19% said they were recommended CBD-only and 17% were recommended high-THC and low-CBD.
Despite this, 44% of patients reported smoking their cannabis, while 34% said they prefer edibles, and nearly one-third (31%) preferred to ingest cannabis extracts or oils. Most patients said they prefer cannabis products that include both THC and CBD, but responses were varied. Twenty-seven percent said they prefer higher levels of THC with lower levels of CBD, while 30% said they preferred higher levels of CBD with lower levels of THC. Twenty-eight percent said they prefer equal levels of both THC and CBD. Only 13% said they prefer a product containing only THC.
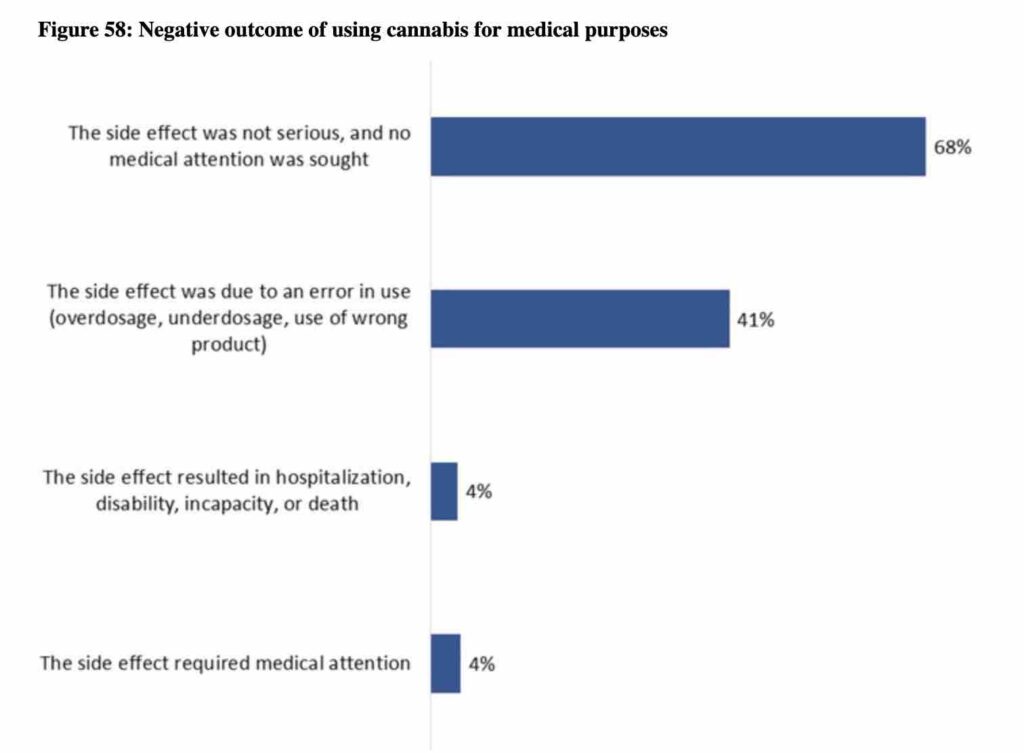
Of those patients who access medical cannabis from a licensed medical cannabis provider, 34% said it is more expensive. More than one quarter (27%) said they found the lack of physical storefronts challenging, while 27% said they could not always get their desired products or had issues with the registration process. Most had no such issues.
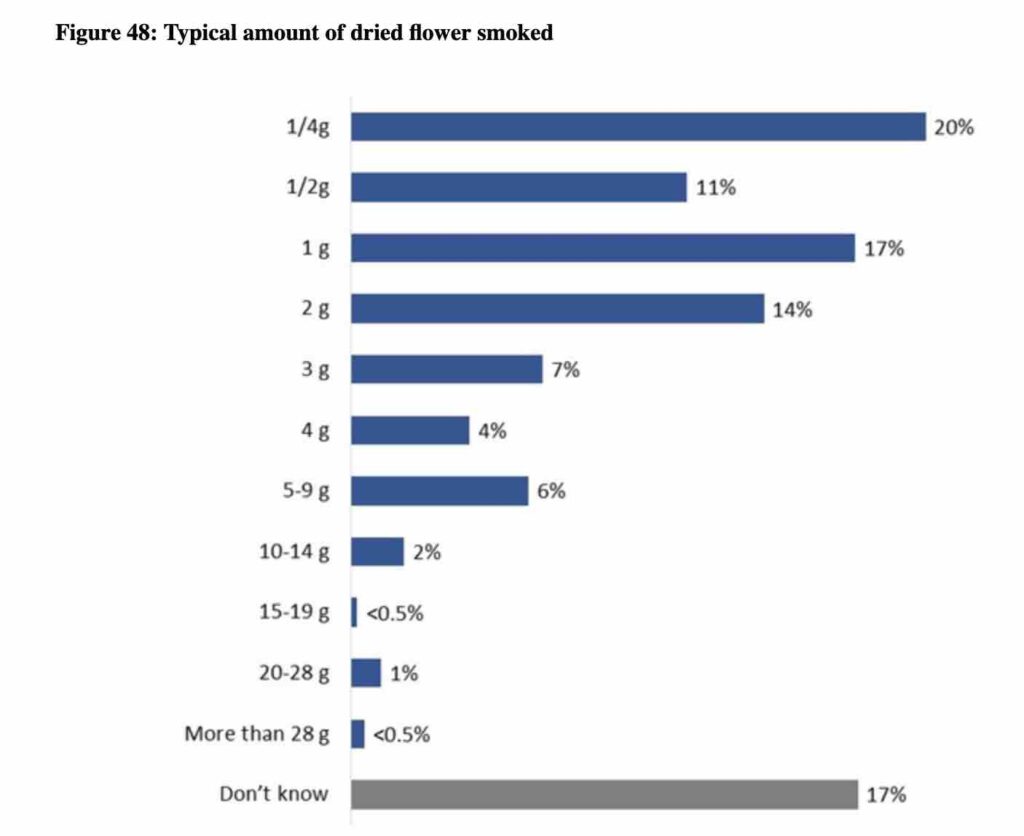
Of those patients who used dried flower, most said they used between .25 grams and 2 grams of cannabis a day. Only 4% reported using more than 10 grams a day. About 17% said they didn’t monitor how much they smoked a day.
Of those who reported vaping cannabis (carts) for medical purposes, nearly one-third (29%) said a cartridge typically lasted them a month. Cartridge size was not noted and can vary typically from half a gram to a gram.
Of those patients who reported dabbing their cannabis, 48% reported using somewhere between 50 and 500 milligrams, while 18% reported using 2 grams or more.
Frequency of use
More than one-third (39%) of those using cannabis for medical purposes said they do so most days, while another 21% said they did so several times a week. Only 14% reported using cannabis for medical purposes once a week, and only 10% reported doing so several times a month.
Sixty percent of patients said they felt legalization had a positive impact on access to cannabis for medical purposes. Of those, about half said they felt full legalization increased the quality and quantity of products, and nearly half reported feeling less stigma for their cannabis use.
Healthcare Practitioner Survey
A second survey also looked into the opinions of healthcare practitioners, with 49% saying there is therapeutic value in the use of cannabis. Another 45% said that there is value at least some of the time.
Of those HCPs who said there is therapeutic value to the use of cannabis at least some of the time, three-quarters cited clinical examples that suggest cannabis can have therapeutic value as their reasoning. Over half (59%) said cannabis was a valuable tool for those instances where other treatment options were not tolerable or effective.
Most (89%) HCPs who felt cannabis has a therapeutic value at least some of the time felt CBD was the most therapeutic part of the plant, while 44% said THC, 13% said other cannabinoids, and 9% said terpenes had therapeutic value.
Most HCPs (90%) said CBD has therapeutic value, while 85% said there were risks associated with THC.
Most HCPs (70%) said they were likely to recommend a legal storefront for access to cannabis for medical purposes, while about 60% reported recommending online access.
Reflecting patient reports, slightly more than half of HCPs (53%) were likely to suggest high-CBD, low-THC products, while 39% recommended CBD-only. Most HCPs (57%) did not give a recommended dose, although those more familiar with cannabis were more likely to do so. Formal authorizations for medical cannabis require a specific amount of cannabis per day, the average being around two grams a day.
Of those who recommend a daily maximum THC dose, the majority recommended no more than 10 mg. The maximum CBD amounts recommended were more varied. About one-third (29%) of HCPs said they typically recommend up to 2.5. mg daily.
The largest single proportion (29%) said they typically recommend up to 2.5 mg of THC daily. Another 22% recommended between 2.6 and 5 mg THC, while 15% typically recommend between 10.1 and 15 mg. Only 1% of HCPs typically recommend more than 25 mg.
Of those HCPs who recommended a daily amount of CBD, 64% typically recommended daily amounts of 10 mg or less, with 27% saying they recommended 5.1 to 10 mg CBD. Thirteen percent said they typically recommended 10.1 and 15 mg, 4% typically recommend between 15.1 and 20 mg, 13% typically recommend between 20.1 and 25 mgs, and only 7% typically recommend more than 25 mg.
Among those who said they typically recommend a daily maximum amount of CBD (n=117), nearly two-thirds (64%) said they typically recommended daily amounts of 10 mg or less, with the largest single proportion (27%) recommending between 5.1 and 10 mg. The proportion of practitioners who typically recommend a daily amount of more than 10 mg includes 13% who typically recommend between 10.1 and 15 mg, 4% who typically recommend between 15.1 and 20 mg, 13% who typically recommend between 20.1 and 25 mg, and 7% who typically recommend more than 25 mg.
Of those HCPs who do not recommend cannabis for medical purposes, most (58%) highlighted a perceived lack of evidence about the efficacy of cannabis or a lack of information about appropriate dosage (55%) to explain why.
Nearly half (48%) said they felt they were not well-informed enough about medical cannabis use or are concerned with negative side effects (47%). Sixty-four percent of HCPs said they have received more requests for information about the use of cannabis for medical purposes since legalization.
Most also said they believe those accessing cannabis for medical purposes are doing so through legal channels compared to prior to full legalization when there was only medical access.
The surveys were conducted by Phoenix Strategic Perspectives Inc. for Health Canada and polled 1,205 Canadians aged 16 and older who have used cannabis for medical purposes since it was legalized on October 17, 2018, and 823 medical doctors and nurse practitioners who have had experiences with patients accessing or inquiring about cannabis for medical purposes since legalization.











